Patients receiving immune-checkpoint inhibitors often experience clinical benefits, but unconventional patterns of response can be observed, emphasising the importance of using a specific approach to evaluating responses to immunotherapy. In an article published in the Nature Reviews Clinical Oncology, the authors review the biological mechanisms underlying the response patterns associated with immune-checkpoint blockade, describe strategies for the assessments of such responses, and highlight the ongoing efforts to identify biomarkers to guide treatment with immune-checkpoint inhibitors.
Cancer immunotherapy using immune-checkpoint blockade has created a paradigm shift in the treatment of advanced-stage cancers. The promising antitumour activity of monoclonal antibodies targeting the immune-checkpoint proteins CTLA-4, PD-1, and PD-L1 led to regulatory approvals of these agents for the treatment of a variety of malignancies.
Patients might experience clinical benefits from treatment with these agents, despite unconventional patterns of tumour response that can be misinterpreted as disease progression, warranting a new, specific approach to evaluate responses to immunotherapy. In addition, biomarkers that can predict responsiveness to immune-checkpoint blockade are being extensively investigated to further advance precision immunotherapy.
In their article, the authors provide state-of-the-art in immune-related response evaluations, identify unmet needs requiring further investigations, and propose future directions to maximize the benefits of immune-checkpoint blockade.
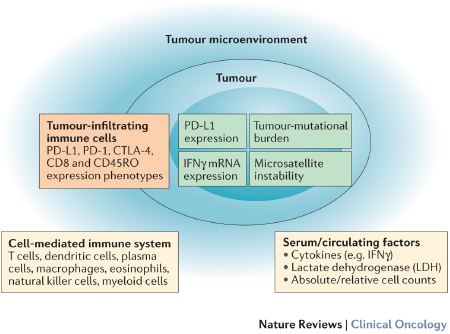
The therapeutic activity of immune-checkpoint inhibitors is the result of a complex interplay between multiple factors in the tumour, tumour microenvironment, and immune system, requiring a collaborative approach to translate the emerging knowledge into the clinical context.
Despite the remarkable success of clinical applications of immunotherapy reported in the past decade, the efficacy and effectiveness of these therapies varies greatly across individual patients and among different tumour types. A substantial unmet need is the development of biomarkers of response to immunotherapeutic agents, in order to identify, before initiation of treatment, which patients are likely to experience a response to and clinical benefit from such treatments.
This aspect is particularly important in the management of tumours with low response rates, such as non-small cell lung cancer (response rate ≤20%), renal-cell carcinoma and urothelial carcinoma, both with response rates ≤30%.
In their article, the authors present the immune-response-associated biomarkers that have been studied to date, discuss their strengths and weaknesses, and highlight ongoing efforts of biomarker development for use in precision cancer immunotherapy. In particular, they discuss about PD-L1 and other immune-checkpoint molecules, tumour-infiltrating lymphocytes, the 'immunoscore' as a biomarker for immunotherapy, mutational burden, neoantigens and microsatellite instability, serum markers and radiographic markers.
They concluded that a development of robust biomarkers to monitor response to immunotherapy is a key next step for the further progress towards precision onco-immunology approaches.
Reference