LUGANO-COPENHAGEN – The PARP inhibitor niraparib significantly improves the outcome of platinum-sensitive recurrent ovarian cancer, according to full data from the ENGOT-OV16/NOVA trial presented for the first time at the ESMO 2016 Congress in Copenhagen and published in the New England Journal of Medicine (NEJM). The trial met its primary endpoint, with niraparib considerably prolonging progression-free survival compared to placebo.
“There are limited treatment options in recurrent ovarian cancer,” said lead author Dr Mansoor Raza Mirza, chief oncologist, Rigshospitalet, Copenhagen University Hospital, Denmark and medical director of the Nordic Society of Gynaecological Oncology (NSGO). “Cumulative toxicity with platinum-based chemotherapy and lack of additional benefit limits its use. We then pause treatment until the next relapse and start combination chemotherapy.”
“The current options for maintenance therapy in the EU are bevacizumab, which can only be given once and improves progression-free survival by just a few months, and the PARP inhibitor olaparib, which is only approved in patients with a germline BRCA mutation (about 10–15% of ovarian cancer patients). No maintenance therapy is approved outside the EU,” he continued.
This phase III trial was performed in collaboration with European Network of Gynaecological Oncology Trial groups (ENGOT). The ENGOT-OV16/NOVA trial evaluated the efficacy and safety of the PARP inhibitor niraparib as maintenance therapy in patients with recurrent ovarian cancer who respond to platinum-based chemotherapy. Patients were assigned to cohorts by BRCA mutation status and randomised 2:1 to receive niraparib 300 mg or placebo once daily.
The trial included 553 patients, of whom 203 had the germline BRCA mutation and 350 did not. Niraparib significantly improved the primary endpoint of progression-free survival compared to placebo in both cohorts, as well as in all subgroups.
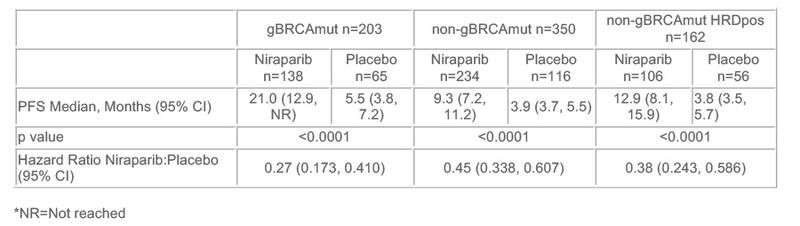
Median progression-free survival with niraparib compared to placebo was 21.0 vs 5.5 months in the germline BRCA mutation group (hazard ratio [HR] 0.27, 95% confidence interval [CI] 0.173 to 0.410, p<0.0001), 9.3 months vs 3.9 months in the non-germline BRCA mutation group (HR 0.45, 95% CI 0.338 to 0.607, p<0.0001), and 12.9 vs 3.8 months in a subgroup of the non-mutation cohort who had homologous recombination DNA repair deficiencies (HRD) (HR 0.38, 95% CI 0.243 to 0.586, p<0.0001).
More than 10% of patients had grade 3/4 adverse events following treatment with niraparib, of whom 28% had thrombocytopaenia, 25% had anaemia, and 11% had neutropaenia. These were resolved with dose adjustments and patients could continue their treatment. Patient-reported outcomes were similar with niraparib and placebo. Patients on niraparib maintained symptom control and had a quality of life comparable to those on placebo.
Significant improvements were also observed in all secondary endpoints. Compared to placebo, niraparib significantly prolonged the second progression-free survival, time to first subsequent treatment, and chemotherapy-free interval in the mutation and mutation-free groups, and in the HRD subgroup.
“This is a breakthrough for patients with ovarian cancer,” said Mirza. “We have never seen such large benefits in progression-free survival in recurrent ovarian cancer. Niraparib significantly improved all endpoints across a broad patient population representing 70% of all ovarian cancer patients. These landmark results could change the way we treat this disease.”
He concluded: “Once it is approved by the regulatory authorities, I’ll consider niraparib for all my patients with recurrent ovarian cancer who respond to platinum regardless of BRCA status.”
Commenting on the results, Dr Andrés Poveda, head of the Gynaecological Cancer Clinic, Oncology Foundation Institute Valencia, Spain, said: “This study more than doubles the population of patients who benefit from a PARP inhibitor.”
“Personalised medicine has arrived in high grade serous ovarian cancer,” he continued. “This was the first trial to use HRD to select patients for treatment and showed that it is a useful strategy. We also know that PARP inhibitors benefit patients with BRCA mutations.”
Poveda concluded: “Future studies are needed to unravel which patients with HRD are not responders to PARP inhibitors and why, and which patients are long responders and why. We also need to know if there are other non-HRD factors, such as cyclin E positivity, that predict which patients will respond to treatment.
-END-
Notes to Editors
References
Abstract LBA3_PR “A randomized, double-blind phase 3 trial of maintenance therapy with niraparib vs placebo in patients with platinum-sensitive recurrent ovarian cancer (ENGOT-OV16/NOVA trial)” will be presented by Dr Mansoor Mirza during the Presidential Symposium 1 on Saturday, 8 October 2016, 16:30 to 18:00 (CEST) in Room Copenhagen.
NEJM citation: Mirza M, Monk B, Herrstedt J, et al. Niraparib maintenance therapy in platinum-sensitive recurrent ovarian cancer. N Engl J Med. DOI: 10.1056/NEJMoa1611310
Disclaimer
This press release contains information provided by the authors of the highlighted abstracts and reflects the content of those abstracts. It does not necessarily reflect the views or opinions of ESMO and ESMO cannot be held responsible for the accuracy of the data. Commentators quoted in the press release are required to comply with the ESMO Declaration of Interests policy and the ESMO Code of Conduct .
About the European Society for Medical Oncology
ESMO is the leading professional organisation for medical oncology. Comprising more than 13,000 oncology professionals from over 130 countries, we are the society of reference for oncology education and information. We are committed to supporting our members to develop and advance in a fast-evolving professional environment.
Founded in 1975, ESMO has European roots and a global reach: we welcome oncology professionals from around the world. We are a home for all oncology stakeholders, connecting professionals with diverse expertise and experience. Our educational and information resources support an integrated, multi-professional approach to cancer treatment. We seek to erase boundaries in cancer care as we pursue our mission across oncology, worldwide.
Abstract for LBA3_PR
A randomized, double-blind phase 3 trial of maintenance therapy with niraparib vs placebo in patients with platinum-sensitive recurrent ovarian cancer (ENGOT-OV16/NOVA trial)
M.R. Mirza1, B.J. Monk2, A. Oza3, S. Mahner4, A. Redondo5, M. Fabbro6, J. Ledermann7, D. Lorusso8, I.B. Vergote9, O. Rosengarten10, J. Berek11, J. Herrstedt12, A.V. Tinker13, A. Dubois14, A. Gonzalez Martin15, P. Follana16, B. Benigno17, B.J. Rimel18, S. Agarwal19, U. Matulonis20
1Department of Oncology 5073, NSGO & Rigshospitalet-Copenhagen University Hospital, Copenhagen, Denmark, 2Department of Oncology, University of Arizona Cancer Center-Phoenix, Phoenix, AZ, USA, 3Department of Oncology, University Health Network, Toronto, ON, Canada, 4Department of Gynegology, AGO & University of Munich, Hamburg, Germany, 5Department of Oncology, GEICO & Hospital Universitario, Madrid, Spain, 6Department of Oncology, GINECO & Institut du Cancer de Montpellier, Montpellier, France, 7Department of Medical Oncology, NCRI & University College London, London, UK, 8Department of Gynecologic Oncology, MITO/MaNGO & Fondazione IRCCS National Cancer Institute, Milan, Italy, 9Department of Obstetrics and Gynecology, BGOG & University of Leuven, Leuven, Belgium, 10Department of Gynecologic Oncology, ISGO & Sha’are Zedek Medical Center, Jerusalem, Israel, 11Department of Oncology, Stanford Women’s Cancer Center, Stanford, CA, USA, 12Department of Oncology, NSGO & Odense University Hospital, Odense, Denmark, 13Department of Medicine, British Columbia Cancer Agency, Vancouver, BC, Canada, 14Department of Oncology, AGO & Kliniken Essen Mitte, Essen, Germany, 15Medical Oncology Department, GEICO & MD Anderson Cancer Center Madrid, Madrid, Spain, 16Department of Medical Oncology, GINECO & Centre Antoine Lacassagne, Nice, France, 17Department of Gynecologic Oncology, University Gynecologic Oncology, Atlanta, GA, USA, 18Department of Obstetrics and Gynecology, Cedars-Sinai Medical Center, West Hollywood, CA, USA, 19Department of Medical Affairs, Tesaro, Inc, Waltham, MA, USA, 20Department of Gynecologic Oncology, Dana-Farber Cancer Institute, Boston, MA, USA
Background: Niraparib is an oral, highly selective inhibitor of PARP1/2. This is the first randomized phase 3 trial of a PARP inhibitor as maintenance therapy post-platinum chemotherapy in patients (pts) with platinum-sensitive recurrent ovarian cancer.
Methods: Two independent cohorts were enrolled based on results of BRACAnalysis® testing: pts with a germline BRCA mutation (gBRCAmut), and pts who lacked these mutations (non-gBRCAmut). Within each cohort, pts were randomized (2:1) to receive niraparib 300 mg or placebo once daily. Three prospectively-defined populations were assessed: 1) the gBRCAmut cohort; 2) those in the non-gBRCAmut cohort whose tumors were retrospectively defined as deficient in homologous recombination (HRD) by the myChoice® HRD test; 3) the overall non-gBRCAmut cohort.
Results: 553 pts were enrolled in this international trial. 60% of pts had 2 lines of prior therapy, and 40% of pts had >2 prior lines. 76% of pts had stage IIIc or IV disease. Niraparib prolonged progression-free survival (PFS) as compared to placebo in all three pt populations (Table 1). Secondary endpoints of chemotherapy-free interval (CFI), time to first subsequent treatment (TFST), and PFS 2 also showed statistically significant improvement. Patient-reported outcomes (PRO) were similar for niraparib and placebo. Most common (≥10%) treatment-emergent grade 3/4 adverse events in niraparib-treated pts were thrombocytopenia (28%), anaemia (25%), and neutropenia (11%). There were no deaths during study treatment.
Conclusions: Niraparib significantly improved PFS for all study populations as well as significantly prolonging CFI, TFST and PFS 2 with a manageable safety profile and without adversely impacting PRO.
Clinical trial identification: NCT01847274
Legal entity responsible for the study: Tesaro Inc.
Funding: Tesaro, Inc.
Disclosure:
B. J. Monk: Consultant for GSK, Merck, Tesaro, Genentech, AZ, Gradalis, Advaxis, Verastem, Cerulean, Amgen, Vermillion, Immunogen, Bayer, NuCana BioMed, Insys Therapeutics, Clovis Oncology, Oxigene, Pfizer – Speaker for Genentech, AZ, Janssen, Myriad Genetics.
A. Oza: Consultant for Amgen, Verastem, Clovis Oncology, Immunovaccine.
S. Mahner: Consultant for Roche, AZ, MSD, Jansen-Cilag, Tesaro, Medac – Honorarium from Roche/Genentech, AZ, PharmaMar, Medac, Jenapharm, Janssen-Cilag, Teva, GSK – Research support from Roche, AZ, BI, GSK, Janssen-Cilag, Medac, PharaMar, Tesaro, Bayer.
A. Redondo: Consultant for Roche, PharaMar – Honorarium from Roche – Speaker for Roche.
M. Fabbro: Has received travel support from Roche.
J. Ledermann: Consultant for AZ/MedImmune, Clovis Oncology – Research support from AZ.
D. Lorusso: Consultant for AZ, PharaMar, Roche Glycart – Speaker for PharmaMar – travel support from PharaMar, Roche Glycart.
I.B. Vergote: Consultant & researcher for AZ, Amgen NV, Array Biopharma, Biogen, BI, BMS, Esai, Lilly, Endocye, Genentech, GSK, Janssen-Cilag, Medimmune, MSD, Morphotek, Nektar, Novo Nordisk, Oasmia, PharaMar, Roche, Sanofi, Shering-Plough, Sigma-Tau, among others.
J. Berek: Consultant for Prima BioMed, Atara Biotherapeutics – Research support from Tesaro, Quest Diagnostics, Endocyte, Genentech, AZ, Prima BioMed.
J. Herrstedt: Consultant for Tesaro.
A.V. Tinker: Consultant for AZ – Research support from AZ/MedImmune.
A. Dubois: Consultant for AZ, PharaMar, Roche/Genentech, Mundipharma, Pfizer.
A. Gonzalez Martin: Consultant for PharaMar, Roche Glycart, - Speaker for AZ, PharaMar, Roche Glycart
P. Follana: Has received travel support from AZ and Roche Glycart.
B. Benigno: Consultant for Genentech – Speaker for and received honorarium from AZ, Insys Therapeutics – Travel support from AZ.
B.J. Rimel: Consultant for AZ – Received Honorarium from Genentech
S. Agarwal: Is an employee of Tesaro.
U. Matulonis: Consultant for Merck KGaA, AZ, Immunogen, Tesaro, Genentech.
All other authors have declared no conflicts of interest.
Keywords: PARP inhibitor, ovarian cancer, Niraparib, maintenance therapy