LUGANO-COPENHAGEN – A phase III trial of sunitinib has met its primary endpoint of disease-free survival for adjuvant treatment of high-risk renal cell carcinoma after nephrectomy, researchers report at the ESMO 2016 Congress in Copenhagen.
“The recurrence rate of kidney cancer after nephrectomy, where part or all of a kidney is removed, is up to 50% in some subgroups of patients,” said lead author Professor Alain Ravaud, head of medical oncology, University Hospital of Bordeaux, France. “This distinguishes it from other tumours such as breast cancer where in general there is a low chance of the cancer coming back.”
“We have good drugs to control disease in patients with metastatic kidney cancer but there are no standard adjuvant treatments,” he added.
This phase III trial tested the ability of adjuvant treatment with sunitinib, a receptor tyrosine kinase inhibitor, to improve disease-free survival in a type of kidney cancer called clear cell renal carcinoma. The study included 615 post-nephrectomy patients at high risk of their cancer recurring. Patients were randomised to placebo or sunitinib for one year. Sunitinib was administered at 50 mg per day in a four weeks on / two weeks off schedule, and one dose reduction to 37.5 mg per day was allowed. Patients with suspected metastases in an independent central review were excluded from the study.
The primary endpoint was disease-free survival. It was assessed by an independent central review committee of radiologists who examined CT scans and ruled whether an event had occurred or not. Events could be recurrence in the remaining kidney or in local lymph nodes, metastases, or a second malignancy. In cases of disagreement between the independent central review and the study investigators a decision was reached by obtaining a biopsy or surgery sample of the tumour – if it contained cancer this was ruled as a recurrence.
The primary endpoint of the trial was met with a significantly longer disease-free survival of 6.8 years with sunitinib compared to 5.6 years with placebo (hazard ratio 0.761, p=0.03). Adverse events of grade 3 or higher were more frequent with sunitinib (62.1%) compared to placebo (21.1%). There were no deaths due to treatment toxicity.
Ravaud said: “Sunitinib is a potential new option for adjuvant therapy in renal cell carcinoma, given the increase in disease-free survival and the manageable safety profile. The results of this trial could change practice because there is currently no standard treatment in this setting.”
He concluded: “We hope sunitinib will be approved by regulators for adjuvant therapy in renal cell carcinoma. Clinicians should then use the drug according to the trial. In other words, in patients with predominant clear cell renal cell carcinoma without metastases and at high risk of recurrence, at a starting dose of 50 mg and a minimum dose of 37.5 mg per day and with the same dosing schedule. This is particularly important since sunitinib was not beneficial in another trial using a different methodology.”
Commenting on the results, Professor Thomas Powles, professor of urology cancer, Barts Cancer Institute, London, UK, said: “This positive trial should be taken in the context of a previous larger adjuvant study (ASSURE) with a very similar design. ASSURE showed no difference in disease-free survival or overall survival. This generates a lot of uncertainty. I suspect a meta-analysis of progression-free survival would be negative and at this point it would be premature to change practice. Both studies show that adjuvant sunitinib is assocated with toxicity.”
He continued: “Disease-free survival is a useful surrogate endpoint, but the results from different studies have been contradictory. It does not necessarily translate to overall survival, which is the gold standard. Preliminary results in this setting do not point towards a survival benefit. There are a number of other trials ongoing in this area and I would like to see one of these being positive to tip the balance towards benefit.”
Powles concluded: “Without a consistently positive disease-free survival signal it would be premature for me to recommend sunitinib as adjuvant therapy for my patients, particularly when one considers the toxicity. A positive survival signal, or meta-analysis for disease-free survival, would be needed. Other studies in this area are awaited.”
-END-
Notes to Editors
References
Abstract LBA11_PR ‘Phase III trial of sunitinib (SU) vs placebo (PBO) as adjuvant treatment for high-risk renal cell carcinoma (RCC) after nephrectomy (S-TRAC)‘ will be presented by Professor Alain Ravaud during the Presidential Symposium 3 on Monday, 10 October 2016, 16:30 to 18:10 (CEST) in Room Copenhagen.
Disclaimer
This press release contains information provided by the authors of the highlighted abstracts and reflects the content of those abstracts. It does not necessarily reflect the views or opinions of ESMO and ESMO cannot be held responsible for the accuracy of the data. Commentators quoted in the press release are required to comply with the ESMO Declaration of Interests policy and the ESMO Code of Conduct .
About the European Society for Medical Oncology
ESMO is the leading professional organisation for medical oncology. Comprising more than 13,000 oncology professionals from over 130 countries, we are the society of reference for oncology education and information. We are committed to supporting our members to develop and advance in a fast-evolving professional environment.
Founded in 1975, ESMO has European roots and a global reach: we welcome oncology professionals from around the world. We are a home for all oncology stakeholders, connecting professionals with diverse expertise and experience. Our educational and information resources support an integrated, multi-professional approach to cancer treatment. We seek to erase boundaries in cancer care as we pursue our mission across oncology, worldwide.
Abstract for LBA11_PR
Phase III trial of sunitinib (SU) vs placebo (PBO) as adjuvant treatment for high-risk renal cell carcinoma (RCC) after nephrectomy (S-TRAC)
Ravaud1, R.J. Motzer2, H.S. Pandha3, M. Staehler4, D. George5, A.J. Pantuck6, A. Patel7, Y-H. Chang8, B. Escudier9, F. Donskov10, A. Magheli11, G. Carteni12, B. Laguerre13, P. Tomczak14, J. Breza15, P. Gerletti16, X. Lin17, M. Lechuga16, J-F. Martini17, J-J. Patard18
1Service d'Oncologie & Radiotherapie, CHU Bordeaux Hopital St. André, Bordeaux, France, 2Department of Medical Oncology, Memorial Sloan Kettering Cancer Center, New York, NY, USA, 3Department of Microbial Sciences, University of Surrey, Surrey, UK, 4Department of Urology, University Hospital of Munich, Munich, Germany, 5Medical Oncology, Duke University, Durham, NC, USA, 6Department of Urology, Ronald Reagan UCLA Medical Center, Los Angeles, CA, USA, 7Oncology, Spire Roding Hospital, London, UK, 8Department of Urology, Taipei Veterans General Hospital, Taipei, Taiwan, 9Medical Oncology, Institut Gustave Roussy, Villejuif, France, 10Department of Oncology, Aarhus University, Aarhus, Denmark, 11Department of Urology, Charité Universitaetsmedizin Berlin, Berlin, Germany, 12Division of Oncology and Division of Urology, 11Azienda Ospedaliera di Rilievo Nazionale A. Cardarelli, Naples, Italy, 13Medical Oncology, Centre Eugene - Marquis, Rennes, France, 14Oncology, Klinika Onkologii Oddzial Chemioterapii, Poznań, Poland, 15Department of Urology, Slovak Medical University in Bratislava, Bratislava, Slovak Republic, 16Oncology, Pfizer S.r.L, Milan, Italy, 17Oncology, Pfizer Inc, San Diego, CA, USA, 18Department of Urology, Bicêtre Hospital, Paris-Saclay University, Le Kremlin Bicetre, France
Background: This randomized, double-blind phase 3 trial examined the efficacy and safety of SU vs PBO in post-nephrectomy patients (pts) with locoregional RCC at high risk (per modified UISS criteria) of tumor recurrence.
Methods: Treatment-naïve pts (n=615) with locoregional RCC (≥T3 and/or N1–2) received 50 mg/d SU or PBO in a 4-wks-on/2-wks-off schedule for 1 yr until disease recurrence, occurrence of secondary malignancy, significant toxicity, or consent withdrawal. One dose reduction to 37.5 mg/d was allowed. Baseline imaging was centrally reviewed to exclude pts with suspicion of metastases. Primary endpoint was disease-free survival (DFS) assessed by central review. Secondary endpoints included investigator-assessed DFS, overall survival (OS), safety, and pt-reported outcomes.
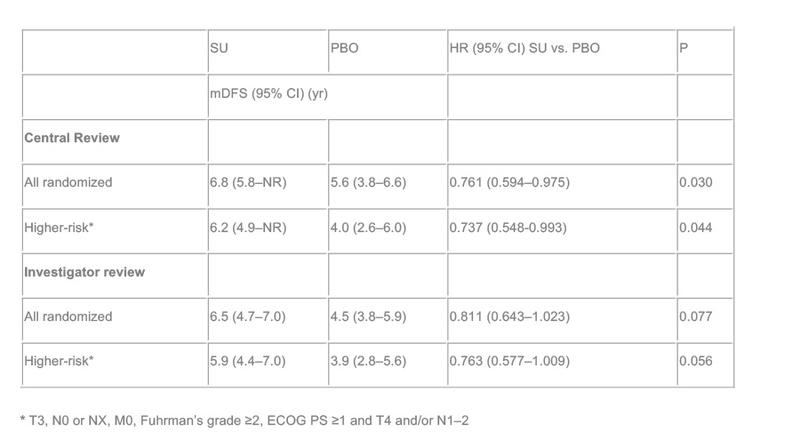
Results: Baseline characteristics were balanced between the SU (n=309) and PBO (n=306) arms. Median (m) number of cycles and relative dose intensity (SU) were 9 and 88.4%, respectively. Fewer DFS events were seen with SU (113; 36.6%) vs PBO (144; 47.1%). The trial met its primary endpoint: DFS by central review was significantly longer for SU vs PBO (HR, 0.761; P=0.030), and these results were supported by secondary DFS analyses in all randomized pts and a higher-risk subgroup (Table 1). OS data were immature at data cutoff (mOS not reached in either arm). Grade ≥3 adverse events (AEs) were more frequent with SU (62.1%) vs PBO (21.1%), but serious AE incidence was similar (21.9% vs 17.1%); no death occurred due to treatment toxicity.
Conclusions: SU prolonged DFS in pts with locoregional RCC at high risk for recurrence. Given the increase in DFS and the manageable safety profile, SU represents a potential new treatment option as adjuvant therapy in RCC.
Clinical trial identification: NCT00375674 (Release date: July 2016)
Legal entity responsible for the study: Pfizer, Inc.
Funding: Pfizer, Inc.
Disclosure:
A. Ravaud: Member of advisory boards in RCC for Pfizer, Novartis, GSK, Roche, and BMS, and received institutional support grants from Pfizer and Novartis, and housing and transportation for meetings and speeches by Pfizer, Novartis, and BMS.
R.J. Motzer: received personal fees and other from Pfizer, Eisai, Novartis, and Exelixis, and other from Bristol Myers Squibb, Genentech/Roche, GlaxoSmithKline, and Acceleron.
M. Staehler: received honoraria, consulting fees, and research grants from Pfizer, Bayer, Novartis, Roche, Bristol Myers Squibb, Aveo, GSK, and Exelixis, and consulting fees from Eisai.
D. George: reports honoraria & consulting: Dendreon, Sanofi, Novartis, Bayer; consulting: Medivation, Merck, Genentech; grants: Genentech/Roche, Novartis, Janssen, Astellas, Celldex, Acerta; grants & consulting: Exelixis, Pfizer, Sanofi, Innocrin Pharma, BMS.
A.J. Pantuck, A. Patel: received consulting fees from Pfizer.
B. Escudier: Received consulting fees from Bayer, Pfizer, and Novartis, and honoraria from Bayer, Roche, Pfizer, Genentech, Novartis, and Aveo.
F. Donskov: Received research funding from Pfizer, Novartis, and GSK.
A. Magheli: Received compensations for speeches from Janssen, Bayer, Astellas, and Pfizer.
B. Laguerre: Received honoraria from Pfizer.
P. Gerletti, X. Lin, M. Lechuga, J-F. Martini: Is an employee of and owns stock in Pfizer Inc.
J-J. Patard: received consulting fees from Pfizer and GSK.
All other authors have declared no conflicts of interest.
Keywords: renal cell carcinoma; tyrosine kinase inhibitor