Results from three trials evaluating the efficacy of different therapeutic combinations that target the human epidermal growth factor receptor 2 (HER2) in patients with HER2-amplified metastatic colorectal cancer (CRC) were reported at the ESMO Congress 2019 in Barcelona, Spain.
Both, TRIUMPH and MOUNTAINEER studies reported high response rates, supporting the strategy of dual HER2 blockade in patients with HER2-amplified metastatic CRC. However, HERACLES-B in patients with metastatic CRC and HER2-amplified tumours did not demonstrate the response rate required by the primary endpoint.
HER2 amplification is a therapeutic target for 2% of unselected patients and up to 6% of patients with RAS wild-type metastatic CRC. All three studies enrolled patients with metastatic CRC and tumours with confirmed HER2 amplification.
Combination of trastuzumab and pertuzumab demonstrated a promising activity in patients with metastatic CRC with RAS wild-type and HER2 amplification confirmed by tissue or ctDNA analysis
In the phase II TRIUMPH study (UMIN000027887) Yoshiaki Nakamura, Department of Gastroenterology and Gastrointestinal Oncology, National Cancer Centre Hospital East in Kashiwa, Japan and colleagues enrolled 19 patients with RAS wild-type and HER2-amplified metastatic CRC that was confirmed by central tissue and/or ctDNA analysis using the Guardant360 assay. Eligible patients had also demonstrated intolerance or were refractory to standard chemotherapy, including anti-epidermal growth fact receptor (EGFR) therapy.
All patients received the HER2 targeted agents trastuzumab plus pertuzumab every 3 weeks. Analysis of the primary endpoint, confirmed objective response rate (ORR) by investigator assessment, was performed separately for tissue-positive patients and for patients who were ctDNA-positive. Each group required a minimum 25 patients for one-sided α = 2.5%, β = 10% to test the threshold ORR of 5% against the expected ORR of 30%. Within these parametres, 5 confirmed responses were needed to determine statistical significance.
Eighteen of the enrolled patients were evaluable for response in the first evaluation. HER2 amplification was confirmed in both tissue and ctDNA samples of 14 patients, in tissue alone for 3, and one patient was confirmed by ctDNA alone, which allowed 17 and 15 patients to be assigned to the tissue-positive and ctDNA-positive group, respectively.
Analysis of the tissue-positive group demonstrated 6 confirmed responses for an ORR of 35% (95% confidence interval [CI], 14-62%). The ORR included one complete response (CR) and 5 partial responses (PR).
In the ctDNA positive group, the ORR was 33% (95% CI, 12-62%), which included one CR and 4 PR.
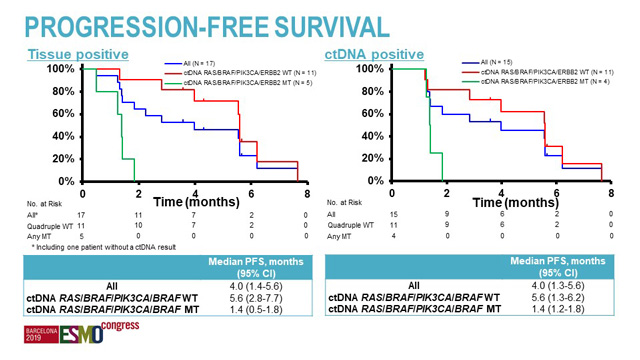
Both arms had the same median progression-free survival (PFS) of 4.0 months (95% CI, 1.4-5.6 months in the tissue positive arm and 95% CI, 1.3-5.6 months in the ctDNA positive arm). The median follow-up was 5.4 months.
All patients with clonal ctDNA mutations in RAS, BRAF, PIK3CA, or HER2 at baseline demonstrated disease progression as best response. The confirmed ORR in patients with wild-type RAS/BRAF/PIK3CA/HER2 in baseline ctDNA was 54.5% (95% CI, 23-83%) in the tissue-positive group, and 45.5% (95% CI, 17-77%) in the ctDNA-positive group, respectively. Patients with wild-type RAS/BRAF/PIK3CA/HER2 in ctDNA also had a higher median PFS than patients with any mutation in RAS/BRAF/PIK3CA/HER2 in ctDNA: 5.6 (95% CI, 2.8-7.7) vs. 1.4 (95% CI, 0.5-1.8) months in the tissue-positive group; 5.6 (95% CI, 1.3-6.2) vs. 1.4 (95% CI, 1.2-1.8) months in the ctDNA-positive group.
With the combination of trastuzumab plus pertuzumab, treatment-related grade 3 decreased ejection fraction and infusion related reaction were reported.
Trastuzumab combined with tucatinib is highly effective in the treatment of patients with RAS wild-type and HER2-amplified metastatic CRC
John H. Strickler, of Duke University Medical Centre in Durham, USA presented initial results from the multicentre open-label single-arm phase II MOUNTAINEER trial (NCT03043313) on behalf of the co-investigators and the Academic and Community Cancer Research United (ACCRU) network.
The incidence of HER2 amplification is higher in patients with RAS wild-type metastatic CRC. Tucatinib is a newly developed potent, highly selective oral tyrosine kinase inhibitor of the HER2 receptor that, in combination with trastuzumab, has demonstrated significantly greater anti-tumour activity compared with either agent alone in patient-derived xenograft models of HER2-positive metastatic CRC, thus providing the rationale for the study.
For inclusion into MOUNTAINEER, patients were required to have RAS wild-type and HER2-amplified metastatic CRC. HER2 amplification and/or overexpression was confirmed in tumour tissue by next generation sequencing (NGS), fluorescent in-situ hybridisation (FISH), or immunohistochemistry (3+ or 2+ and amplified by FISH). Patients were also required to have received prior treatment with 5-FU, oxaliplatin, irinotecan, and an anti-VEGF antibody; patients receiving anti-HER2 therapy previously were excluded.
Of the 26 enrolled patients, 62% were male with a median age of 50 years (range, 24 to 70 years). The primary tumour site of origin was the right colon in 4 patients, left colon or rectum in 17 patients, transverse colon in 3 patients, and overlapping/ multiple sites in 2 patients.
Patients were treated with oral tucatinib at 300 mg twice daily and standard doses of trastuzumab per i.v. every 3 weeks. The primary endpoint was ORR per RECIST v1.1. The study used a 2-Stage Fleming design to compare ORR of 20% (null) to 40% (alt) in 10 or 25 evaluable patients using a 1-sided α= 0.11; β=0.16, which required at least 8 responses to meet the primary efficacy endpoint.
As of 26 April 2019, 26 patients enrolled and 23 patients completed ≥1 evaluation of response and were evaluable. Among these patients, the ORR was 52%, which included 12 CR/PR with an additional 6 patients experiencing stable disease (SD); 5 patients had disease progression. The median duration of response was not reached.
The clinical benefit rate, defined as CR plus PR plus SD that was maintained ≥4 months, was 64%.
Median PFS was 8.1 months (95% CI, 3.8-not estimated [NE]). Median overall survival was 18.7 months (95% CI, 12.3-NE).
Two (8%) patients had grade 3 treatment-related adverse events (TRAEs), but there were no grade 4/5 TRAEs. The most common TRAEs included grade 1 AST and ALT elevations in 38% and 23% of patients, respectively. Grades 1, 2, and 3 diarrhoea were reported in 4%, 15%, and 4% of patients, respectively.
Pertuzumab plus T-DM1 does not show enhanced objective response while providing disease control in RAS wild-type, HER2-amplified, metastatic CRC
Andrea Sartore-Bianchi and colleagues, of Niguarda Cancer Center and University of Milano, Italy, were the first to show with the HERACLES-A multicentre clinical trial that a dual blockade of HER2 is effective in metastatic CRC patients with tumours harbouring amplification of this oncogene, providing ORR as high as 30% with the combination of trastuzumab and lapatinib.
Based on this, the open-label phase II HERACLES-B study (EudraCT number 2012-002128-33) has been launched, evaluating a targeted chemotherapy approach with a combination of pertuzumab and T-DM1 in patients with RAS/BRAF wild-type, HER2-amplified metastatic CRC. Eligible patients had performance status 0-1 and showed disease progression following treatment with 5-FU, oxaliplatin, irinotecan, and anti-EGFR containing regimens; the patients had received a median of 3 prior regimens.
All patients were treated with pertuzumab at 840 mg per i.v. load, followed by 420 mg i.v. every 3 weeks and T-DM1 at 3.6 mg/kg every 3 weeks. NGS-based molecular analyses of tumour tissue and plasma samples were performed.
The ORR served as the primary endpoint and PFS was the secondary endpoint. The study used a Fleming/Hern design (H0 = ORR 10%; α = 0.05; power = 0.85), which required 7 (30%) patients to demonstrate either a PR or CR.
Of the 30 patients enrolled from August 2016 to March 2018, all were evaluable for efficacy by the time data lock and centralised radiological revision were completed.
At data cut-off, the ORR was 10% (95% CI, 40-28%) and 70% (95% CI, 50-85) of patients showed SD, while median PFS was 4.8 months (95% CI, 3.6-5.8), which compared favourably to the historical median PFS of 4.2 months reported in HERACLES-A.
Therefore, the majority of patients with RAS/BRAF wild-type HER2-positive metastatic CRC did not show enhanced ORR but achieved SD and prolonged PFS following targeted therapy with combined pertuzumab and T-DM1.
Higher HER2 expression by immunohistochemistry score (3+ versus 2+) was associated with greater ORR and SD lasting ≥4 months (p = 0.03).
A total of 296 treatment cycles were delivered. Grade ≤2 adverse events occurred in 84% of cycles, which consisted primarily of mainly nausea and fatigue. TRAEs grade 3 adverse events of thrombocytopenia were observed in 2 patients.
Conclusions
TRIUMPH and MOUNTAINEER studies met their respective primary efficacy endpoint of ORR.
The TRIUMPH study is the first trial to prospectively evaluate the efficacy of dual HER2-blockade for metastatic CRC with HER2 amplification by tissue or ctDNA analysis, and demonstrated promising activity with the combination of trastuzumab plus pertuzumab in patients with treatment-refractory metastatic CRC with HER2 amplification in tissue and/or ctDNA. Furthermore, the authors concluded the combination has an acceptable toxicity profile that is consistent with previous reports for each agent. They noted further that clonal oncogenic ctDNA driver mutations, such as KRAS, BRAF, PIK3CA, or HER2 may predict for primary resistance to treatment.
The MOUNTAINEER trial demonstrated promising activity for tucatinib and trastuzumab, with more than half of evaluable patients with RAS wild-type and HER2-amplified metastatic CRC achieving an objective response. The study combination was well tolerated as well. These results suggest that further expansion of the MOUNTAINEER trial in patients with HER2-amplified metastatic CRC is warranted.
Although HERACLES-B did not reach its primary endpoint (ORR), the authors noted that disease control (PR plus SD) was achieved in 80% of patients with a median PFS of 4.8 months that favourably compares to the median 4.2 months achieved in the positive HERACLES-A trial. They proposed that the ORR may have been weakened by the lower trastuzumab dose delivered with T-DM1, while the longer PFS could be the result of the combined ‘broad-brush’ effect of emtansine and synergy with pertuzumab.
Disclosure
The TRIUMPH study was funded by the Japan Agency for Medical Research and Development. The MOUNTAINEER trial was funded by Seattle Genetics and supported through the ACCRU network. The HERACLES-B is a non-profit clinical trial sponsored by Fondazione Piemontese per l'Oncologia - FPO funded by Associazione Italiana per la Ricerca sul Cancro (AIRC); Roche provided pertuzumab and T-DM1 for free.
References
526PD – Nakamura Y, Okamoto W, Kato T, et al. TRIUMPH: Primary Efficacy of a Phase II Trial of Trastuzumab (T) and Pertuzumab (P) in Patients (pts) with Metastatic Colorectal Cancer (mCRC) with HER2 (ERBB2) Amplification (amp) in Tumor Tissue or Circulating Tumor DNA (ctDNA): A GOZILA Sub-study.
527PD – Strickler JH, Zemla T, Ou F-S, et al. Trastuzumab and tucatinib for the treatment of HER2 amplified metastatic colorectal cancer (mCRC): Initial results from the MOUNTAINEER trial.
LBA35 – Sartore-Bianchi A, Martino C, Lonardi S, et al. Phase II Study of Pertuzumab and Trastuzumab-emtansine (T-DM1) in Patients with HER2-positive Metastatic Colorectal Cancer: the HERACLES-B (HER2 Amplification for Colo-rectaL cancer Enhanced Stratification, cohort B) Trial.